New course on healthy cat ownership
Invisible’s new continuing medical education course, “Zoonotic diseases and pet cats,” describes common diseases that can…

Invisible’s new continuing medical education course, “Zoonotic diseases and pet cats,” describes common diseases that can…

In our newly released medical education course, a Dublin-based infectious disease physician-researcher raises the alarm about…

As 2022 comes to an end, the team at Invisible International is taking a moment to…

Bridging the Knowledge Gap Between Human and Animal Clinicians Register: https://tinyurl.com/y3285t6m When: Nov. 5, 2022 —9am…
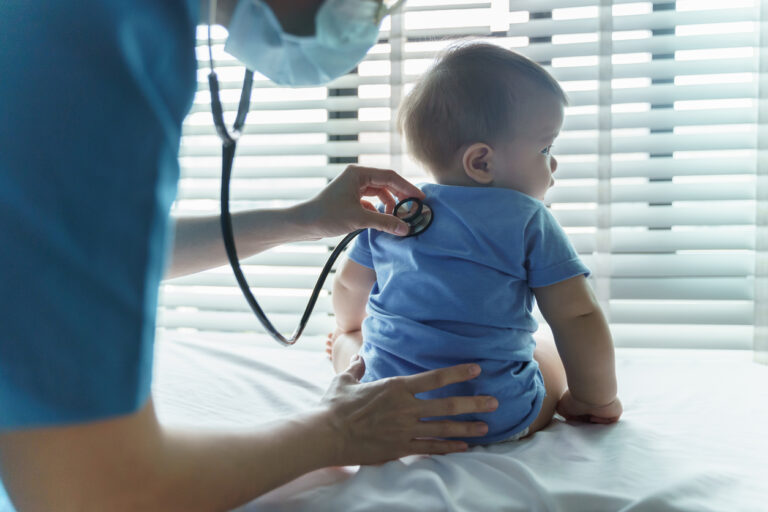
Lyme disease affects children more than any other age group, but the young ones are often…
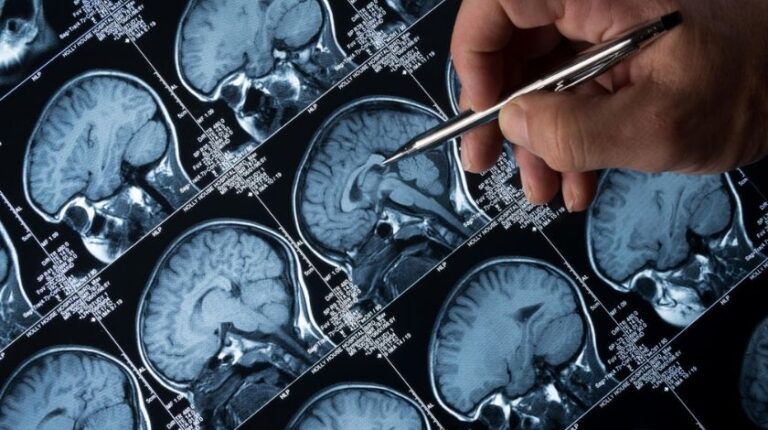
Invisible International has released a new course on neurological and neuropsychiatric manifestations of Bartonella, a family…

In this free medical education course, Kenneth Liegner, MD, a New York-based internist who has been…

Monica Embers, PhD, director of the vector-borne disease research center at Tulane University School of Medicine,…

A retrospective study of 270 post-treatment Lyme patients identified the most debilitating neurological symptoms, paving the way for…

Two tick-borne disease experts, a physician and a researcher, discuss the many ways Lyme bacteria evade the immune…
End of content
End of content